Weight Management
thumbnail
Supplement Regulations
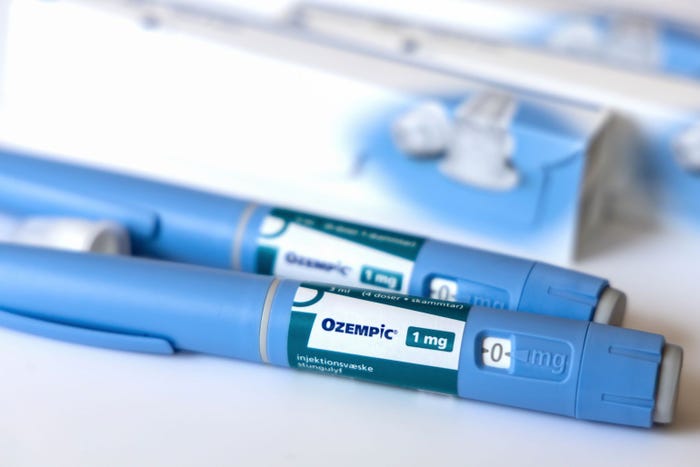
‘Vague’ NY law looms for The Vitamin Shoppe, other supplement retailers‘Vague’ NY law looms for The Vitamin Shoppe, other supplement retailers
With New York Assembly Bill A5610 set to take effect in less than two weeks, manufacturers and retailers are gearing up to comply with its requirements.
Subscribe and receive the latest insights on the health and nutrition industry.
Join 37,000+ members. Yes, it's completely free.












.png?width=300&auto=webp&quality=80&disable=upscale)




























.png?width=800&auto=webp&quality=80&disable=upscale)