Proteins
thumbnail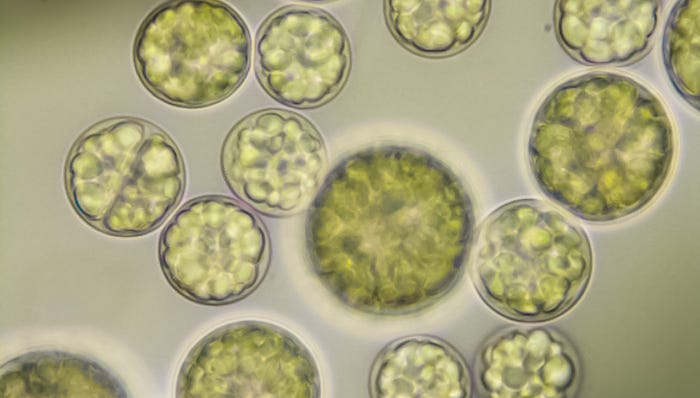
Healthy Living
Aker enters protein space, announces new algal DHA ingredientAker differentiates ingredient mix with algal DHA, marine protein
Krill oil specialist Aker BioMarine is bringing to market an algal DHA ingredient. The raw material, which is extracted in its Houston facility, comes from a partner. Aker is also developing a protein ingredient at a pilot plant in Norway.
Subscribe and receive the latest insights on the health and nutrition industry.
Join 37,000+ members. Yes, it's completely free.






























































.png?width=800&auto=webp&quality=80&disable=upscale)