Fat-soluble vitamin K is essential for proper blood clotting, bone mineralization and vascular health; however, certain drugs can have adverse effects on bioavailability and activity, and taking in the most biological active form can help ensure optimal health effects.
April 18, 2011

Vitamin K, also known as menadione, phylloquinone, menaquinones or antihemorrhagic factor, is chemically a group of fat-soluble 2-methyl-1,4-naphthoquinone derivatives. All members of the vitamin K group of vitamins share a methylated naphthoquinone ring structure and vary in the aliphatic side chain attached at the 3-position. The fat-soluble vitamin is carried through the body by lipids and stored in fat tissue. The "K" is derived from the German word "koagulation." Coagulation refers to the process of blood clot formation. The existence of the vitamin K group was discovered by Henrik Dam in 1929, while studying cholesterol metabolism in chicks; he was awarded the 1943 Nobel Prize for the discovery. Vitamin K is cofactor of VK-dependent carboxylation reactions in a number of biochemical pathways. Vitamin K is essential for the functioning of several proteins involved in blood clotting, bone mineralization, vascular health and cell growth. As with other lipid-soluble vitamins, a normal flow of bile and pancreatic enzymes is necessary with the presence of dietary fat to enhance absorption.
There are two basic types (forms) of vitamin K.
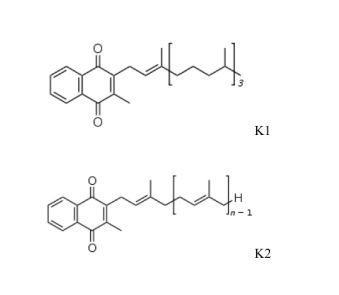
Vitamin K1, known as phylloquinone (phytonadione/phytomenadione), is probably the most important dietary source for humans. It is considered natural, being synthesized by plants, and is concentrated in leafy greens and other green vegetables. When humans or animals consume vitamin K1, their tissues convert part of it into vitamin K2. It is the trans-isomer (not cis-) form that is biologically active.
Vitamin K2 consists of the menaquinone (MK) forms MK-3 through MK-14. The various forms of K2 are differentiated by having side chains lengths composed of a variable number of unsaturated isoprenoid units; generally they are designated as MK-n, where n specifies the number of isoprenoids (side chain) attached to the napthoquinone ring.
The menaquinones are mainly of microbial origin in the gut, and are also converted from vitamin K1 in the body. It currently is thought the important dietary menaquinones range from MK-4 through MK-10. MK-3 is a vitamin precursor of K2, but is primarily created synthetically as a toxic alkylating agent and is banned from use in dietary supplements by FDA. At this time, the two primary menaquinones being commercially sold for human nutrition are MK-4 and MK-7.
MK-4 appears to be synthesized by animals (including humans) from K1 and can be commercially manufactured synthetically. MK-4 is found in a number of organs other than the liver at higher concentrations than K1. This fact, along with the existence of a unique pathway for its synthesis, suggests MK-4 has a unique biological function that has not yet been identified. MK-4 can even activate blood clotting factors, which is a role traditionally given to vitamin K1. It appears to remain active in the body only a few hours.
MK-7 is considered superior to vitamin K1 in several important areas, including better absorption, much longer bioavailability and higher efficacy levels in the body. It is made in large amounts by the bacterium Bacillus subtilis that ferments the Japanese condiment called natto. MK-7 stays in the circulation for longer than MK-4 in humans; a three-day half-life in the blood, compared to the one- to two-hour half-life of K1.
Human studies show vitamin K2 is absorbed up to 10 times more than K1 and remains biologically active in the body far longer than K1. For instance, K1 is rapidly cleared by the liver within eight hours, whereas measurable levels of K2 have been detected 72 hours after ingestion.
Biological Functions
Vitamin K is essential for the activation of vitamin K-dependent proteins, which involve blood coagulation, bone metabolism and the inhibition of arterial calcification.
Vitamin K is a necessary cofactor for normal clotting of blood in humans. Specifically, vitamin K is required for the liver synthesis of the coagulation proteins making the clotting factors that are necessary for blood to properly coagulate. These factors are: factor II (prothrombin), factor VII (proconvertin), factor IX (thromboplastin component) and factor X (Stuart factor). The mechanism by which vitamin K promotes formation in the liver of clotting factors II, VII, IX and X is not fully understood. Other anticoagulation clotting factors that depend on vitamin K are proteins C, S and Z. Deficiency of vitamin K or disturbances of liver function (for example, severe liver failure) may lead to deficiencies of these clotting factors, causing excess bleeding.
For calcium/bone health, vitamin K has a key function primarily as an essential co-factor for the enzyme gamma-glutamyl-carboxylase (GGCX), responsible for gamma-carboxylation (synthesis) of vitamin K-dependent proteins. Two of these involved in calcium and bone metabolism are osteocalcin and matrix Gla-protein (MGP). Vitamin K plays a critical role in maintaining healthy bone density by facilitating the transport of calcium from the bloodstream into the bone.
Vitamin K is also required by calcium-regulating proteins in the arteries (vascular system). MGP is a vitamin K-dependent protein and must be carboxylated to function properly; poor vitamin K blood levels result in synthesis of uncarboxylated MGP (ucMGP). Since MGP is a potent local inhibitor of arterial calcification, MGP is important in relation to the health of the entire cardiovascular system. Without adequate vitamin K, calcium in the blood can bind to the arterial wall resulting in calcification. Arterial calcification has also been found to decrease bone mineralization (bone loss), often called the calcification paradox. It is observed mainly in patients with osteoporosis and chronic kidney disease.
Adequate Intake, Deficiencies
Under normal conditions, vitamin K is moderately well absorbed (40 percent to 70 percent) from the jejunum and ileum, but very poorly in the colon. Vitamin K deficiency is rare, but can result from lack of vitamin K in the diet or from intestinal disorders that impair fat absorption, reducing absorption. Deficiency may occur in patients with biliary obstruction or other conditions limiting absorption of vitamin K such as celiac disease, ulcerative colitis, sprue, regional enteritis, cystic fibrosis, intestinal resection, and in patients receiving drugs that may affect liver function or intestinal flora. Vitamin K deficiency may also weaken bones.
Vitamin K deficiency can develop in people who take certain drugs, including anticoagulants, as vitamin Ks pro-clotting actions can work against this type of medicine. Warfarin and other 4-hydroxycoumarin derivatives are antagonists of vitamin K action and are effective antithrombotic agents. Vitamin K blocks the conversion of KO (vitamin K-epoxide) into K by inhibiting the enzyme KO reductase. A patient who is treated with Warfarin or other 4-hydroxycoumarin derivatives should refrain from taking vitamin K, without consultation with his doctor or pharmacist. However, vitamin K does not counteract the anticoagulant effect of heparin. The use of broad spectrum antibiotics, quinidine, quinine and high-dose salicylates may also increase requirements for vitamin K.
Newborns are prone to vitamin K deficiency because only small amounts of vitamin K cross the placenta and because, during the first few days after birth, their intestines do not contain bacteria to produce vitamin K. The deficiency can cause hemorrhagic disease of the newborn (hypoprothrombinemia), characterized by a tendency to bleed. A vitamin K injection is usually administered to newborns to protect them from this issue. Breast-fed infants who have not received this injection at birth are especially susceptible to deficiency because breast milk contains only small amounts of vitamin K.
The main symptom of vitamin K deficiency is bleeding (hemorrhage)the delayed, slowed or inability for the flowing blood to clot. Having a liver disorder also increases the risk of bleeding because proteins that help blood clot (clotting factors) are made in the liver. One routine test used to check this is the Prothrombin time (PT) or International Normalized Ratio (INR) test, which measures the time required for blood to clot. A result showing a delayed clot formation may indicate a deficiency of vitamin K. The same test is often used on patients taking blood-thinners to determine the correct drug dosage required.
Studies suggest although dietary vitamin K intake levels are adequate for normal blood clotting, they may be insufficient overall. The present dietary reference values for vitamin K are based on proper functioning of blood coagulation only. The Recommended Daily Allowance (RDA) for vitamin K is:
Age | Children | Men | Women |
0-6 months | 2.0 mcg/d | NA | NA |
7-12 months | 2.5 mcg/d | NA | NA |
1-3 years | 30 mcg/d | NA | NA |
4-8 years | 55 mcg/d | NA | NA |
9-13 years | 60 mcg/d | NA | NA |
14-18 years | 75 mcg/d | NA | NA |
19-71+ years | NA | 120 mcg/d | 90 mcg/d |
NOTE: RDA/AI levels are no different for pregnant and lactating women than the general population recommendations.
Robin Koon, senior vice president at Best Formulations , has more than 25 years of pharmaceutical experience in clinical pharmacy, as a drug chain executive overseeing operations and managed-care and in retail mass market.
About the Author(s)
You May Also Like




.png?width=800&auto=webp&quality=80&disable=upscale)